
Correlations between Higher-Order Aberrations and Astigmatic Degree
Abstract
We aimed to investigate the correlations between the astigmatic axis and higher-order aberrations (HOAs) and between astigmatic degrees and HOAs within a specific range of myopic degrees.
The HOAs of 992 eyes were analyzed with a LADARWave device using a Hartmann-Shack system. The astigmatic degree and axis were determined through a manifest refraction test.
The differences in most vertical aberrations between non-astigmatic and against-the-rule (ATR) astigmatic eyes were greater than those between non-astigmatic and with-the-rule (WTR) or oblique astigmatic eyes. The largest differences between non-astigmatic and WTR astigmatic eyes were observed in vertical second-order astigmatism and vertical quadrafoil aberrations. By contrast, the most pronounced differences between non-astigmatic and oblique astigmatic eyes were found in coma and oblique trefoil aberrations. When the correlation between astigmatic degree and HOAs was evaluated, WTR astigmatic eyes showed significant relationships with vertical coma, vertical trefoil, vertical second-order astigmatic, and vertical quadrafoil aberrations. Similarly, oblique astigmatic eyes exhibited significant correlations with vertical trefoil, oblique trefoil, and vertical second-order astigmatism aberrations. Conversely, no significant correlations were observed between astigmatic degree and HOAs. Vertical coma aberration increased significantly with higher WTR astigmatic degrees in eyes with myopic degrees of −3.00D or less and −3.00 D ≤ −6.00.
HOAs varied based on the astigmatic axis, whereas the correlation between astigmatic degree and HOAs was influenced by the astigmatic axis and myopic degree.
초록
난시축과 고차수차(HOA)와의 상관관계, 그리고 근시도 분류에 따른 난시도와 고위수차 사이의 상관관계를 조사하였다.
Hartmann-Shack 시스템을 적용한 LADARWave 장치를 이용하여 총 992안의 고위수차를 분석하였고, 현성굴절검사를 통해 굴절이상과 난시축을 측정하였다.
대부분의 수직수차는 난시가 없는 눈과 도난시 사이에서 난시가 없는 눈과 직난시와 사난시 사이의 차이보다 더 컸다. 그리고 난시가 없는 눈과 직난시안의 차이는 수직 2차 난시 및 수직 트레포일수차에서 가장 컸다. 구면수차와 오블리크 트레포일수차는 난시가 없는 눈과 사난시 사이에서 가장 큰 차이를 보였다. 난시도와 고위수차 사이의 상관관계를 분석할 때, 직난시안은 수직 코마, 수직 트레포일, 수직 2차 난시 및 수직 콰드라포일수차와 유의한 상관관계가 있었다. 사난시안은 수직 트레포일, 오블리크 트레포일 및 수직 3차 난시수차와 유의한 상관관계가 있었지만, 도난시안은 고위수차와와 통계적으로 유의한 상관관계가 없었다. 수직 코마수차는 근시도 −3.00 D 이하와 −3.00< D ≤−6.00에서 직난시가 증가함에 따라 유의하게 증가하였다.
본 연구를 통해 고위수차는 난시축에 따라 달라지는 것으로 나타났으며, 난시도와 고위수차의 상관관계는 난시축과 근시도에 영향을 받는 것으로 나타났다.
Keywords:
Hartmann-Shack, Higher-order aberration, Astigmatic axis, Astigmatic degree, Myopic degree키워드:
고위수차, 난시축, 난시도, 근시도Introduction
With the increasing awareness of higher-order aberrations (HOAs) that cannot be corrected with prescription glasses, numerous studies have been conducted to understand these aberrations and develop strategies to reduce them. During the twentieth century, mathematical representation of HOAs using the Zernike polynomial became possible.[1-3]
Generally, optical aberrations are classified into lower-order aberrations (myopia, hyperopia, and astigmatism) and HOAs. Lower-order aberrations can be corrected using contact lenses, refractive surgeries with excimer lasers, and vision correction surgeries, such as cataract surgeries. By contrast, HOAs refer to visual distortions that persist even after the correction of ametropia.[4-6] First- and second-order aberrations are categorized as lower-order aberrations, whereas third-, fourth-, and above-order aberrations are classified as higher-order aberrations.[ 3,4] HOAs that cannot be corrected by prescription glasses and are known to increase aberrations after laser vision correction surgery compromise vision quality.[7-12]
Aberration measurement methods include the Hartmann-Shack technique,[1] Tscherning or ray tracing technique,[ 13] and Eye Mapper.[14] Among these, the Hartmann-Shack technique has gained popularity in recent years. This method employs a lenslet array of micro-lenses created by boring multiple holes into a transparent disc, through which parallel rays in a ray bundle move straight toward the retina. When the rays deflected by the retina return, a distorted wavefront is generated due to the divergence of the light traveling toward and through the retina.[1] HOAs are measured using the value of this divergence, calculated through the Zernike polynomial.[2-4]
The introduction of wavefront devices capable of measuring HOAs has significantly advanced the field, facilitating their use in surgeries to minimize aberrations and in predicting visual acuity following the implantation of intraocular lenses (IOLs). Most previous studies on HOAs have focused on postsurgical outcomes, including investigations into changes in HOA levels after laser-assisted in situ keratomileusis surgery[7-12] or phakic IOL (pIOL) implantations,[15] postsurgical comparisons of HOAs between pIOL implantations and refractive surgeries,[16] changes in HOAs after cataract surgeries,[17] and changes in HOAs that are dependent on the surgical incision size in cataract surgeries.[18-20] Moreover, studies have found correlations between specific HOAs and refractive errors and various factors, such as age-dependent changes.[21-23] However, HOAs are influenced by multiple interacting factors rather than a single determinant. This complexity makes it challenging to predict the overall visual quality based solely on the correlations between a single factor, such as age, myopia, or astigmatism, and HOAs. Therefore, analyses controlling for the effects of complex variables are necessary.
In this study, analyses were conducted to explore the correlations between the astigmatic degree/axis and HOAs and the changes in HOAs that were dependent on the astigmatic degree. These investigations aimed to elucidate the correlation between complex lower-order aberrations and HOAs.
Materials and Methods
1. Study Participants
The study included 496 Korean individuals aged 20– 62 years (male:female=240 eyes:652 eyes) with a maximum correction visual acuity of >1.0 and no corneal or retinal disease. The participants’ mean age was 33.3±8.8 years, the mean degree of myopia was −4.93±2.36 D (range: −0.37 to −12.00 D), and the astigmatic degree was −1.24±1.10 D (range: 0 to −5.75 D). The participants refrained from wearing soft lenses for more than 1 week, toric soft lenses for more than 2 weeks, and hard lenses for more than 3 weeks.
To analyze the changes in HOAs based on the degrees of myopia and astigmatism, the participants’ eyes were classified as follows: non-astigmatic eyes (astigmatic degree = 0D), with-the-rule (WTR) astigmatic eyes, against-the-rule (ATR) astigmatic eyes, and oblique astigmatic eyes (Table 1).
To analyze the correlation between WTR astigmatism and HOAs at specific myopic degrees, the participants’ eyes were divided into the following groups based on myopic degree: 0.00 D < Group M1 ≤ −3.00 D, −3.00 D < Group M2 ≤ −6.00 D, −6.00 D < Group M3 ≤ −9.00 D, and −9.00 D < Group M4 ≤ −12.00 D. Similarly, to analyze the correlations between ATR astigmatism and HOAs, the participants’ eyes were divided into 0.00 D < Group M5 ≤ −3.00D, and −3.00D < Group M6 ≤ −6.00 D based on the myopic degree (Table 1).
2. Aberration Measurement
Aberrations were measured using the LADARWave system (Alcon Laboratories, Inc., Fort Worth, Texas, USA) following the Hartmann-Shack technique. The measurements were taken at a 6.5 mm optical zone under controlled lighting conditions, with laboratory illumination set at 27 lux and illumination on the patient’s eye at 8 lux. Aberrations were assessed following the application of a cycloplegic agent.
3. Manifest Refraction Test
A manifest refraction test was performed using an experimental lens set and a system chart (SC-2000, NIDEC Corporation, Kyoto, Japan). The visual acuity test laboratory was illuminated at 7 lux, whereas illumination on the patient’s eye during the acuity test was maintained at 8 lux. Refractive errors, including myopic degree (measured in 0.12 D increments) and astigmatic degree (measured in 0.25 D increments), were determined using a trial lens set and a cross-cylinder method.
4. Statistical Analyses
A simple linear regression analysis was performed using SPSS (version 12.0, IBM Corporation, Armonk, NY, USA), and the results were expressed as the mean ±standard deviation. A bivariate correlation analysis was conducted, and the strength of the correlation was assessed using the values of r. A P value of less than 0.05 was considered significant.
Results and Discussions
1. Dependence of HOAs on the astigmatic axis
Among the 992 participants’ eyes, 90 (9.1%) had 0D astigmatism, 688 (69.4%) had a WTR astigmatism, 130 (13.1%) had an ATR astigmatism, and 84 (8.5%) had an oblique astigmatism. Regardless of the myopic status or axis, coma aberrations were the largest, followed by spherical, vertical trefoil, vertical coma, and horizontal coma aberrations (Table 2).
When non-astigmatic and WTR astigmatic eyes were compared, the vertical second-order astigmatic aberration of WTR astigmatic eyes was 270.2% greater than that of non-astigmatic eyes, whereas the horizontal coma aberration was 44.2% smaller. When non-astigmatic eyes were compared with ATR astigmatic eyes, the differences in HOAs-except for spherical aberration, oblique second-order astigmatism, and vertical second-order astigmatism aberration-were larger than those observed between non-astigmatic and WTR astigmatic eyes. The comparison between non-astigmatic and oblique astigmatic eyes showed that the differences in coma, spherical, vertical trefoil, and vertical quadrafoil aberrations were less than 20%, whereas the differences in the rest of the aberrations were substantial (Table 2).
For each HOA, coma aberration remained consistent across different astigmatism types. The vertical coma aberration of WTR astigmatic eyes was greater than that of non-astigmatic eyes, whereas those of ATR or oblique astigmatic eyes were relatively smaller; the largest difference was observed in ATR astigmatic eyes. The horizontal coma aberration of WTR, ATR, and oblique astigmatic eyes was smaller than that of non-astigmatic eyes, with the largest difference observed in ATR astigmatic eyes. The oblique trefoil aberration in oblique astigmatic eyes was the largest, which was more than six times greater than that in ATR astigmatic eyes. Vertical quadrafoil aberration was largest in non-astigmatic eyes and smallest in WTR astigmatic eyes (Table 2).
2. Correlation between astigmatic degree and HOAs
For WTR astigmatisms, coma, vertical coma, horizontal coma, and oblique trefoil aberrations showed a positive correlation with increasing astigmatic degree, whereas vertical trefoil, spherical, vertical second-order astigmatic, oblique second-order astigmatic, oblique quadrafoil, and vertical quadrafoil aberrations exhibited a negative correlation. Among them, the changes in vertical coma (r=−0.091, p=0.08), vertical trefoil (r=0.069, p=0.034), vertical second-order astigmatic (r=0.102, p=0.004), and vertical quadrafoil aberrations (r=0.109, p=0.002) were significant (Table 2, Fig. 1).
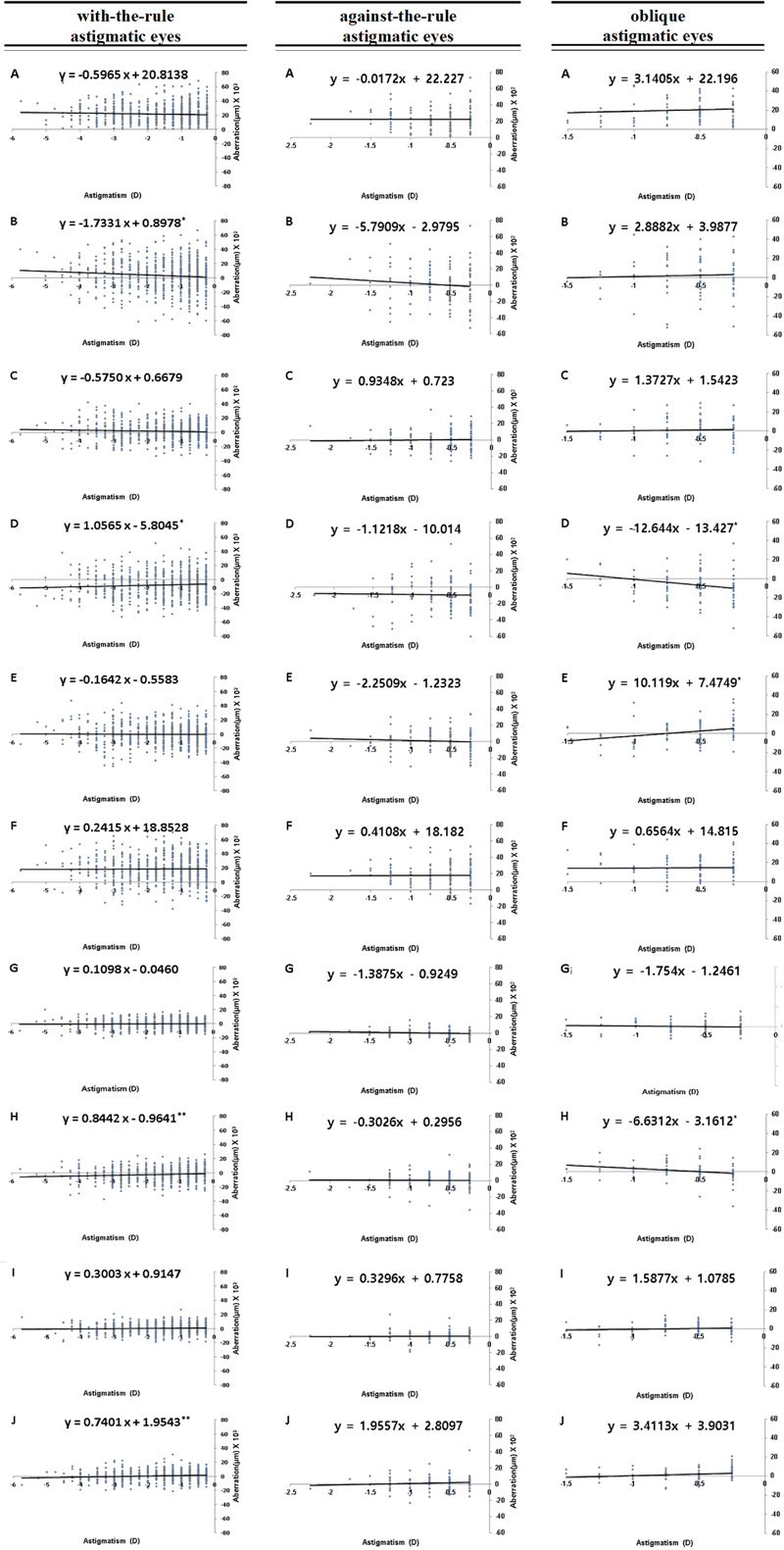
The correlation between astigmatism and higher-order aberrations classified based on astigmatic axis in a 6.5 mm pupil diameter. (A) Coma aberration. (B) Vertical coma aberration (Z3−1). (C) Horizontal coma aberration (Z31). (D) Vertical trefoil aberration (Z3−3). (E) Oblique trefoil aberration(Z33). (F) Spherical aberration (Z40). (G) Oblique second-order astigmatism aberration (Z4−2). (H) Vertical second-order astigmatism aberration (Z42). (I) Oblique quadrafoil aberration (Z4−4). (J) Vertical quadrafoil aberration (Z44). The slope of the trend lines represent the regression line with the best linear fit, with the asterisk showing the significant levels: *p<0.05;**p<0.01.
For ATR astigmatic eyes, coma, vertical coma, vertical trefoil, oblique trefoil, oblique second-order astigmatic, and vertical second-order astigmatic aberrations showed a positive correlation with increasing astigmatic degree, whereas other aberrations exhibited a negative correlation. However, these changes were not significant (Table 2, Fig. 1).
For oblique astigmatic eyes, vertical trefoil, oblique second-order astigmatic, and vertical second-order astigmatic aberrations showed a positive correlation with increasing astigmatic degree, whereas the other aberrations showed a negative trend. Among these, the changes in vertical trefoil (r=−0.246, p=0.012), oblique trefoil (r=0.269, p=0.007), and vertical second-order astigmatic aberrations (r=−0.237, p=0.015) were significant (Table 2, Fig. 1).
3. Correlation between astigmatic degrees and HOAs in a certain range of myopic degrees
For WTR astigmatic eyes, the slope of the trend line for the association between astigmatic degree and coma aberration was −1.6381 in Group M1, which had the least astigmatismand significantly increased as the astigmatic degree increased (rM4=−0.149, pM4=0.047). However, no significant correlation was found in other astigmatic groups (Fig. 2).
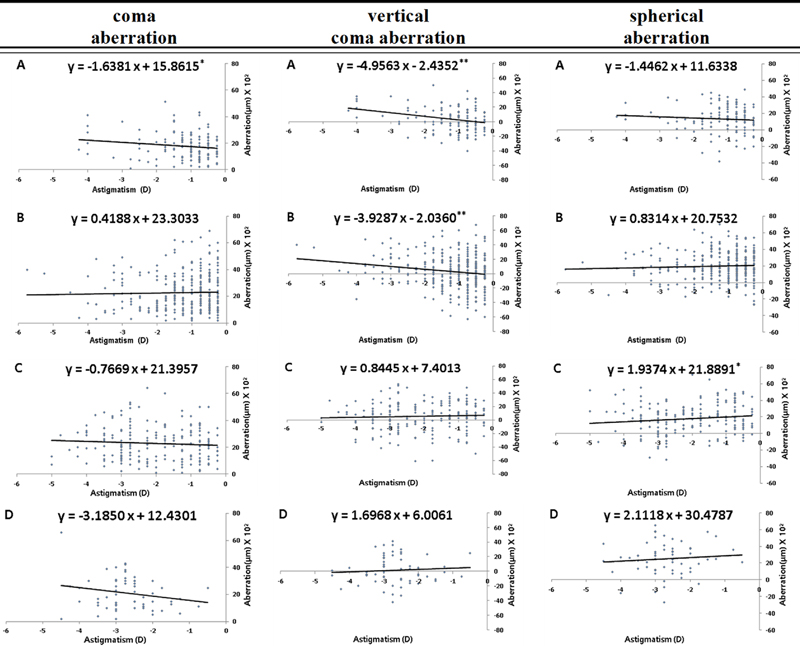
The correlation between astigmatism and higher-order aberrations classified by myopic degree in a 6.5 mm pupil diameter. (A) Myopic degree of −0.00 < D ≤ −3.00. (B) Myopic degree of −3.00 < D ≤ −6.00. (C) Myopic degree of −6.00 < D ≤ -9.00. (D) Myopic degree of −9.00 < D ≤ −12.00. The slope of the trend lines represent the regression line with the best linear fit, with the asterisk showing the significant levels: *p<0.05; **p<0.01.
The trend line slopes expressing the relationship between the astigmatic degree and vertical coma aberration were −4.9563 and −3.9287 for Group M1 and Group M2, respectively, indicating a positive increase in aberration as the astigmatic degree increased. This increase was considered significant (rM1=−0.273, pM1=0.001; rM2=−0.163, pM2=0.002). However, the trend line slopes were 0.8445 (rM3=0.047, pM3=0.261) in Group M3 and 1.6968 (rM4=0.073, pM4=0.291) in Group M4, demonstrating a change in the correlation between astigmatic degree and vertical coma aberration as the degree of myopia increased (Fig. 2).
The trend line slopes for spherical aberration were −1.4462 for Group M1, 0.8314 for Group M2, 1.9374 (r=0.125, p=0.043) for Group M3, and 2.1118 for Group M4. This indicates an increasing trend of spherical aberrations in the negative direction as the myopic degree increased (Fig. 2).
For vertical trefoil aberration, the trend line slope in Group M1 was 4.1165 and significantly decreased as WTR astigmatism increased (rM1=0.242, pM1=0.003), whereas the trend line slope in Group M4 was −11.1618, showing a significant increase (rM4=−0.485, pM4<0.0001) (Fig. 3).
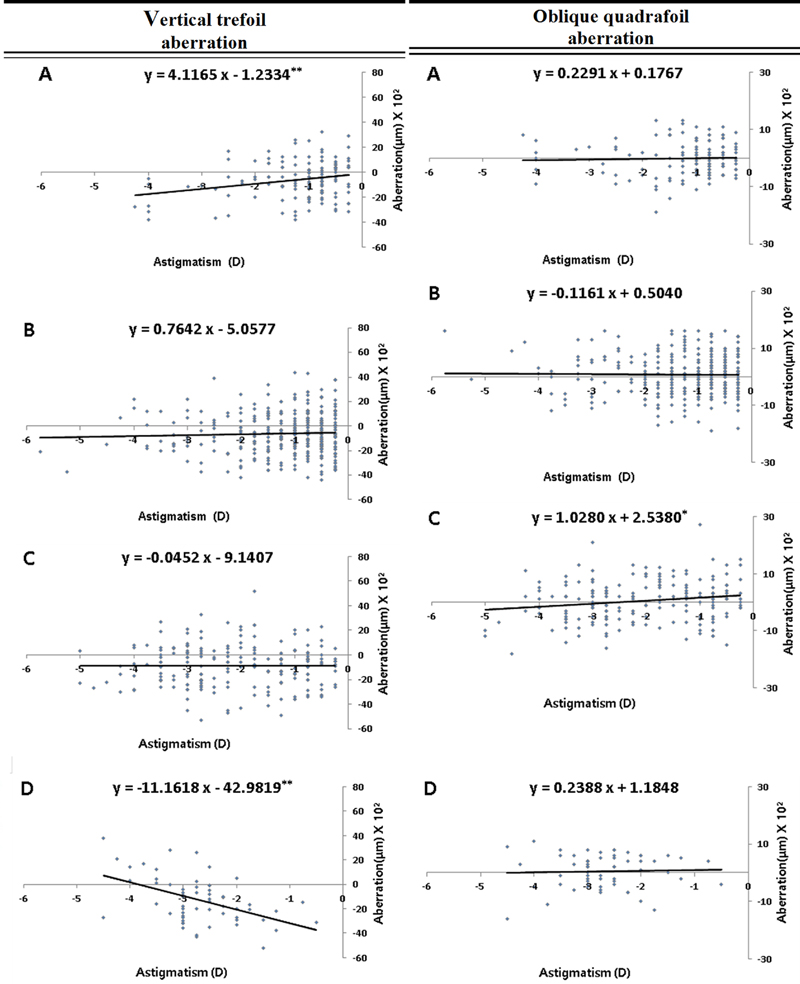
The correlation between astigmatism and higher-order aberrations classified by myopic degree in a 6.5-mm pupil diameter. (A) Myopic degree of −0.00 < D ≤ −3.00. (B) Myopic degree of −3.00 < D ≤ −6.00. (C) Myopic degree of −6.00 < D ≤ −9.00. (D) Myopic degree of -9.00 < D ≤ −12.00. The slope of the trend lines represent the regression line with the best linear fit, with the asterisk showing the significant levels: *p<0.05; **p<0.01.
For oblique quatrefoil aberration, the trend line slope in Group M3 was 1.0280, showing a correlation where the aberration significantly decreased as WTR astigmatism increased. However, the change in aberration due to increased astigmatism was not large (rM4=0.168, pM4= 0.010), and no significant changes were observed in other astigmatic groups (Fig. 3).
4. Correlation between ATR astigmatic degree and HOAs within a certain range of myopic degrees
No consistent correlation was found between the astigmatic degree and aberrations that were dependent on the myopic degree for the other aberrations.
As the majority of ATR astigmatic eyes had a myopic degree of less than −6.00 D (55 eyes in Group M5, 65 eyes in Group M6, and 10 eyes in other groups), only Groups M5 and M6 were analyzed. Although no significant correlations were observed between the astigmatic degree and coma, horizontal coma, or spherical aberrations in either group, the trend lines for the correlation between astigmatic degree and vertical coma aberration showed a slope of −15.925 (rM6=−0.259, pM6=0.019), whereas that between astigmatic degree and oblique second-order astigmatism showed a slope of −3.689 (rM6=−0.246, pM6=0.024). Both of these results indicated a significant increase in the aberration as the astigmatic degree increased (Table 3).

Correlation between astigmatism and high-order aberration of against-the-rule astigmatic eyes according to myopic degree in a 6-mm pupil diameter
Due to the limited number of participants, oblique astigmatic eyes were not analyzed (Table 1).
HOAs are primarily induced by the cornea and lens. Although corneal aberrations contribute significantly to coma and spherical aberrations, third-order and higher-order aberrations are corrected by complementary lens aberrations.[24] The delicate balance and regulation between the cornea and lens determine the overall quality of vision. Any disruption in this balance can alter vision quality. Various factors can affect this equilibrium, including recent vision correction surgeries,[7-12] pIOL implantation,[15-20] use of rigid gas permeable contact lenses,[25,26] refractive error,[21,24,27,28] aging,[22,23] dry eye syndrome,[29-32] pupil size,[2] accommodation,[33-36] keratoconus,[37,38] and corneal type.[39] Applegate et al.[40] reported that the delicate balance of aberration correction can be disrupted, leading to changes in the eye’s aberration structure following surgeries that alter vision quality.
Moreover, studies have shown that irregularities in the tear film increase over time after blinking, which can elevate third- and fourth-order aberrations, limiting vision improvement after corneal abrasions.[29] This highlights how minor changes in the cornea can significantly affect HOAs and, consequently, vision quality. Additionally, Guirao et al.[19] found that temporal and nasal incisions during cataract surgery led to changes in the astigmatic degree (0.7 D for temporal incisions and 1.5 D for nasal incisions), accompanied by an increase in trefoil aberrations -most prominent in WTR astigmatic eyes. However, no changes were noted in coma and spherical aberrations. This suggests that HOAs can be influenced by corneal limbal incisions, and the resulting aberrations vary depending on the type of incision.
Changes in HOAs can be caused by a variety of factors and are influenced by various variables. Several studies have explored the factors associated with HOAs, such as the correlation between myopic eye and HOAs, [21,24,27,28] the correlation between age and HOAs,[22,23] the comparison of HOAs based on pupil size and accommodation stimulus,[33,34] the correlation between accommodation and spherical aberration,[35,36] and the correlation between HOAs and simple refractive error. [5,23,28] However, most of these studies analyzed the correlations based on a single factor, without accounting for the effects of other contributing variables. To address this limitation, the present study examined how the correlations between the astigmatism degrees and HOAs were affected by the astigmatic axis. Compared with non-astigmatic eyes, WTR astigmatic eyes exhibited larger vertical coma aberrations, whereas ATR and oblique astigmatic eyes showed smaller vertical coma aberrations. Horizontal coma aberration was smaller in WTR, ATR, and oblique astigmatic eyes than in non-astigmatic eyes. Additionally, the spherical aberration was largest in WTR astigmatic eyes and smallest in oblique astigmatic eyes, indicating that HOAs vary depending on the astigmatic axis.
Kwan et al. [5] reported that spherical aberration is significantly correlated with refractive error and decreases as myopia increases. However, the results of the present study showed that spherical aberration decreased as the degree of astigmatism increased across WTR, ATR, and oblique astigmatic eyes. In the low myopia group (0.00 D < Group M1 ≤ −3.00 D), spherical aberration increased as the degree of astigmatism increased. This suggests that the change in spherical aberration differs between groups with high and low degrees of myopia. In other words, spherical aberration was influenced by the degree of astigmatism, which is a lower-order aberration, in conjunction with myopia.
As for the correlation between the degree of astigmatism and HOAs, an increasing trend in coma, vertical coma, and oblique trefoil aberrations was observed as the astigmatic degree increased in WTR and ATR astigmatic eyes. In ATR and oblique astigmatism, the aberrations showing a positive correlation with increasing astigmatic degree included vertical trefoil, oblique second-order astigmatism, and vertical second-order astigmatism. No aberration exhibited a simultaneous positive correlation across all types of astigmatism (WTR, ATR, and oblique). However, spherical, oblique quadrafoil, and vertical quadrafoil aberrations showed an increasing trend in the negative direction in all types of astigmatic eyes. This suggests that the correlation between astigmatism and HOAs was influenced by the astigmatic axis. Karimian et al.[21] reported a significant correlation between myopic astigmatic eyes and oblique trefoil, spherical, and vertical coma aberrations, which contradicted the results of this study. As the study by Karimian et al.[21] was conducted on a Middle Eastern population (Iranians), anatomical and physiological differences, potentially due to racial factors, might account for the discrepancy. Additionally, the sample size in that study was smaller (123 eyes) compared with the 992 eyes examined in this study. Moreover, only a specific range of myopic eyes was selected in that study. These differences are likely the reason for the variation in the results compared with those of this study.
HOAs are affected not only by the degree of astigmatism but also by the degree of myopia. Therefore, excluding the effects of myopic degrees is necessary to accurately determine the effect of the astigmatic degree. In this study, the correlations between the degrees of astigmatism and HOAs were investigated within a specific range of myopic degrees to minimize the effects of myopic degrees.
The eye groups within a specific range of myopic degrees were compared to exclude the influence of myopic degrees. For WTR astigmatic eyes, a significant correlation between the degree of astigmatism and vertical coma aberration was only observed in the group with a myopic degree of less than −3.00 D and the group with myopic degrees of more than −3.00 D but less than −6.00 D. For ATR astigmatic eyes, a significant correlation was found in the group with myopic degrees of more than −3.00 D but less than −6.00 D. These findings suggest that HOAs were affected by both myopic and astigmatic degrees, which are lower-order aberrations. Furthermore, vertical coma aberration was most strongly affected by myopic degrees, indicating a likely correlation between vertical coma aberration and vision quality, which was dependent on the astigmatic degrees.
A previous study by Leung TW et al.[39] examined the correlation between astigmatic degree and HOAs by comparing a simple myopic group with an ATR myopic astigmatism (MA) group. Their study found that the MA group exhibited significantly more negative HOAs for vertical trefoil aberration and more positive HOAs for vertical coma aberration. This finding is similar to the results of our study, where the mean aberration was compared between a group without astigmatism and a group with ATR astigmatism. The ATR astigmatism group showed more negative HOAs for vertical trefoil aberration and more positive HOAs for vertical coma aberration. However, the mean size of HOAs reported in the study by Leung TW et al.[39] differed significantly from that in our study. Leung TW et al.[39] examined 46 elderly participants (mean age, 50-70 years), with 28 participants comprising the simple myopic group (spherical-equivalent refractive error (M) ≦ −0.50D, astigmatism (Cyl) ≦ 0.75) and 18 participants comprising the MA group (M ≦ −0.50, Cyl ≧ 1.00, minus cylinder correcting axis equal to 90±20 degrees).
In our study, the astigmatism axis, astigmatic degree, age range, sample size, and measurement and analytical methods differed from those in the previous study.[39] These methodological differences between the studies may explain the variations in the mean aberration results. Additionally, in our study, the aberrations were compared not only in the ATR astigmatism group but also in the WTR and oblique astigmatism groups, among participants without astigmatism. However, these findings should be confirmed in future studies that include larger sample sizes of participants with ATR astigmatism and oblique astigmatism. By analyzing the potential impact of myopia degree on the correlation between astigmatic degree and HOAs, our study provides a more precise examination of the effects of astigmatic degree on HOAs compared with previous studies.[4,21,24,27,28,33,39]
Conclusions
This study presented valuable data on the correlations between the astigmatic degrees and HOAs. Given the increasing exposure to environments that can disrupt tear film stability, such as the frequent use of various media or communication devices along with procedures that can affect the astigmatic degree (e.g., vision correction surgery, cataract surgery, and IOL implantation), the results of this study on the correlation between the astigmatic degree and HOAs are expected to serve as foundational research material. These findings may contribute to developing solutions to improve vision quality.
Acknowledgments
본 논문의 일부 내용은 2012학년도 한국안광학회 동계학술대회에서 구연으로 발표되었음.
References
-
Liang J, Grimm B, Goelz S, et al. Objective measurement of wave aberrations of the human eye with the use of a Hartmann-Shack wave-front sensor. J Opt Soc Am A Opt Image Sci Vis. 1994;11(7):1949-1957.
[https://doi.org/10.1364/JOSAA.11.001949]

-
Paquin MP, Hamam H, Simonet P. Objective measurement of optical aberrations in myopic eyes. Optom Vis Sci. 2002;79(5):285-291.
[https://doi.org/10.1097/00006324-200205000-00007]

-
Guirao A, Williams DR, Cox IG. Effect of rotation and translation on the expected benefit of an ideal method to correct the eye's higher-order aberrations. J Opt Soc Am A Opt Image Sci Vis. 2001;18(5):1003-1015.
[https://doi.org/10.1364/JOSAA.18.001003]

-
Collins MJ, Wildsoet CF, Atchison DA. Monochromatic aberrations and myopia. Vision Res. 1995;35(9):1157-1163.
[https://doi.org/10.1016/0042-6989(94)00236-F]

-
Kwan WC, Yip SP, Yap MK. Monochromatic aberrations of the human eye and myopia. Clin Exp Optom. 2009;92(3):304-312.
[https://doi.org/10.1111/j.1444-0938.2009.00378.x]

-
Yoon G, Jeong TM, Cox IG, et al. Vision improvement by correcting higher-order aberrations with phase plates in normal eyes. J Refract Surg. 2004;20(5):S523-S527.
[https://doi.org/10.3928/1081-597X-20040901-22]

- Moreno-Barriuso E, Lloves JM, Marcos S, et al. Ocular aberrations before and after myopic corneal refractive surgery: LASIK-induced changes measured with laser ray tracing. Investig Ophthalmol Vis Sci. 2001;42(6):1396-1403.
-
Reed DS, Apsey D, Steigleman W, et al. Retrospective analysis of the post-operative changes in higher-order aberrations: a comparison of the WaveLight EX500 to the VISX S4 laser in refractive surgery. Mil Med. 2017;182 (11-12):e2061-e2065.
[https://doi.org/10.7205/MILMED-D-17-00159]

-
Wang J, Ren Y, Liang K, et al. Changes of corneal high-order aberrations after femtosecond laser-assisted in situ keratomileusis. Medicine. 2018;97(18):e0618.
[https://doi.org/10.1097/MD.0000000000010618]

-
Smadja D, Santhiago MR, Mello GR, et al. Corneal higher order aberrations after myopic wavefront-optimized ablation. J Refract Surg. 2013;29(1):42-49.
[https://doi.org/10.3928/1081597X-20121210-03]

-
Jin HY, Wan T, Wu F, et al. Comparison of visual results and higher-order aberrations after small incision lenticule extraction (SMILE): high myopia vs. mild to moderate myopia. BMC Ophthalmol. 2017;17(1):118.
[https://doi.org/10.1186/s12886-017-0507-2]

-
Xu Y, Yang Y. Small-incision lenticule extraction for myopia: results of a 12-month prospective study. Optom Vis Sci. 2015;92(1):123-131.
[https://doi.org/10.1097/OPX.0000000000000451]

-
Piñero DP, Sánchez-Pérez PJ, Alió JL. Repeatability of measurements obtained with a ray tracing aberrometer. Optom Vis Sci. 2011;88(9):1099-1105.
[https://doi.org/10.1097/OPX.0b013e3182223788]

-
Fedtke C, Ehrmann K, Falk D, et al. The BHVI-EyeMapper: peripheral refraction and aberration profiles. Optom Vis Sci. 2014;91(10):1199-1207.
[https://doi.org/10.1097/OPX.0000000000000364]

-
Hashemian SJ, Farrokhi H, Foroutan A, et al. Ocular higher-order aberrations changes after implantable collamer lens implantation for high myopic astigmatism. J Curr Ophthalmol. 2018;30(2):136-141.
[https://doi.org/10.1016/j.joco.2017.10.002]

-
Shin JY, Ahn H, Seo KY, et al. Comparison of higher order aberrations after implantable collamer lens implantation and wavefront-guided LASEK in high myopia. J Refract Surg. 2012;28(2):106-111.
[https://doi.org/10.3928/1081597X-20111018-02]

- Rajabi MT, Korouji S, Farjadnia M, et al. Higher order aberration comparison between two aspherical intraocular lenses: MC6125AS and Akreos advanced optics. Int J Ophthalmol. 2015;8(3):565-568.
-
Alió JL, Elkady B, Ortiz D. Corneal optical quality following sub 1.8 mm micro-incision cataract surgery vs. 2.2 mm mini-incision coaxial phacoemulsification. Middle East Afr J Ophthalmol. 2010;17(1):94-99.
[https://doi.org/10.4103/0974-9233.61225]

-
Guirao A, Tejedor J, Artal P. Corneal aberrations before and after small-incision cataract surgery. Investig Ophthalmol Vis Sci. 2004;45(12):4312-4319.
[https://doi.org/10.1167/iovs.04-0693]

-
Song IS, Park JH, Park JH, et al. Corneal coma and trefoil changes associated with incision location in cataract surgery. J Cataract Refract Surg. 2015;41(10):2145-2151.
[https://doi.org/10.1016/j.jcrs.2015.10.052]

- Karimian F, Feizi S, Doozande A. Higher-order aberrations in myopic eyes. J Ophthalmic Vis Res. 2010;5(1):3-9.
-
Wei S, Song H, Tang X. Correlation of anterior corneal higher-order aberrations with age: a comprehensive investigation. Cornea. 2014;33(5):490-496.
[https://doi.org/10.1097/ICO.0000000000000099]

-
Wan XH, Li SM, Xiong Y, et al. Ocular monochromatic aberrations in a rural Chinese adult population. Optom Vis Sci. 2014;91(1):68-75.
[https://doi.org/10.1097/OPX.0000000000000107]

-
Artal P, Guirao A. Contributions of the cornea and the lens to the aberrations of the human eye. Opt Lett. 1998;23(21):1713-1715.
[https://doi.org/10.1364/OL.23.001713]

-
Choi J, Wee WR, Lee JH, et al. Changes of ocular higher order aberration in on- and off-eye of rigid gas permeable contact lenses. Optom Vis Sci. 2007;84(1):42-51.
[https://doi.org/10.1097/01.opx.0000254036.45989.65]

-
Berntsen DA, Barr JT, Mitchell GL. The effect of overnight contact lens corneal reshaping on higher-order aberrations and best-corrected visual acuity. Optom Vis Sci. 2005;82(6):490-497.
[https://doi.org/10.1097/01.opx.0000168586.36165.bb]

-
He JC, Sun P, Held R, et al. Wavefront aberrations in eyes of emmetropic and moderately myopic school children and young adults. Vision Res. 2002;42(8):1063-1070.
[https://doi.org/10.1016/S0042-6989(02)00035-4]

-
Cheng X, Bradley A, Hong X, et al. Relationship between refractive error and monochromatic aberrations of the eye. Optom Vis Sci. 2003;80(1):43-49.
[https://doi.org/10.1097/00006324-200301000-00007]

-
Montés-Micó R, Alió JL, Muñoz G, et al. Postblink changes in total and corneal ocular aberrations. Ophthalmology. 2004;111(4):758-767.
[https://doi.org/10.1016/j.ophtha.2003.06.027]

-
Koh S, Maeda N. Wavefront sensing and the dynamics of tear film. Cornea. 2007;26:S41-S45.
[https://doi.org/10.1097/ICO.0b013e31812f69e8]

-
Koh S, Maeda N, Hirohara Y, et al. Serial measurements of higher-order aberrations after blinking in patients with dry eye. Investig Ophthalmol Vis Sci. 2008;49(1):133-138.
[https://doi.org/10.1167/iovs.07-0762]

-
Denoyer A, Rabut G, Baudouin C. Tear film aberration dynamics and vision-related quality of life in patients with dry eye disease. Ophthalmology. 2012;119(9):1811-1818.
[https://doi.org/10.1016/j.ophtha.2012.03.004]

-
Buehren T, Collins MJ, Carney LG. Near work induced wavefront aberrations in myopia. Vision Res. 2005;45(10):1297-1312.
[https://doi.org/10.1016/j.visres.2004.10.026]

- Wu WJ, Zhang ZP, Qian YY, et al. Changes in monochromatic higher-order aberrations in different pupil sizes with accommodation in young emmetropes. Zhonghua Yan Ke Za Zhi. 2008;44(7):603-608.
-
Theagarayan B, Radhakrishnan H, Allen PM, et al. The effect of altering spherical aberration on the static accommodative response. Ophthalmic Physiol Opt. 2009;29(1):65-71.
[https://doi.org/10.1111/j.1475-1313.2008.00610.x]

-
Hazel CA, Cox MJ, Strang NC. Wavefront aberration and its relationship to the accommodative stimulus-response function in myopic subjects. Optom Vis Sci. 2003;80(2):151-158.
[https://doi.org/10.1097/00006324-200302000-00011]

-
Jinabhai A, O'Donnell C, Tromans C, et al. Optical quality and visual performance with customised soft contact lenses for keratoconus. Ophthalmic Physiol Opt. 2014;34(5):528-539.
[https://doi.org/10.1111/opo.12133]

-
Ortiz-Toquero S, Rodriguez G, de Juan V, et al. Repeatability of placido-based corneal topography in keratoconus. Optom Vis Sci. 2014;91(12):1467-1473.
[https://doi.org/10.1097/OPX.0000000000000421]

-
Leung TW, Lam AKC, Kee CS. Ocular aberrations and corneal shape in adults with and without astigmatism. Optom Vis Sci. 2015;92(5):604-614.
[https://doi.org/10.1097/OPX.0000000000000581]

-
Applegate RA, Marsack JD, Ramos R, et al. Interaction between aberrations to improve or reduce visual performance. J Cataract Refract Surg. 2003;29(8):1487-1495.
[https://doi.org/10.1016/S0886-3350(03)00334-1]

