Correlation between Axis-Rotation and Corneal Topography in Toric Soft Contact Lens Fitting
Abstract
Purpose: This study aimed to investigate the effects of different corneal topographies on the rotation of toric soft contact lenses.
Toric soft contact lenses were fitted to 107 with-the-rule astigmatic eyes in patients aged 20–39 years who presented oval, symmetric bow tie, or asymmetric bow tie corneal shapes based on the Bogan classification method. The changes in lens rotation patterns due to blinking were assessed, along with the patterns of lens rotation for 1 min following changes in the direction of gaze or after rotating the lens 45°.
The extent of axial rotation of toric lenses during primary gaze exhibited statistically significant differences depending on the corneal topography, wherein asymmetric bow tie-shaped corneas had the largest rotation. In the diagonal gaze, statistically significant differences in the amount of rotation were observed for all corneal shapes. Moreover, although oval-shaped corneas demonstrated significant differences in the horizontal gaze, symmetric and asymmetric bow tie-shaped corneas revealed significant differences only in the vertical gaze. When the lens was arbitrarily rotated 45° in the temporal direction, there were no differences in rotation patterns between the different corneal shapes. After rotation in the temporal to nasal direction, there were no differences for up to 45 s, but differences were observed in the 45–60 s interval.
As corneal topography demonstrably affects the amount of rotation of toric soft contact lenses, corneal shape should be taken into consideration during lens fitting to ensure optimal axial stability.
초록
본 연구는 각막 지형 형태에 따른 토릭 소프트 콘택트렌즈의 회전 특성을 분석하고, 각막 지형이 렌즈 회전에 미치는 영향을 규명하고자 하였다.
Bogan 분류법에 따라 타원형(oval), 대칭나비형(symmetric bow tie), 비대칭 나비형(asymmetric bow tie) 각막 지형을 가지고 있는 20-39세의 직난시(with-the-rule astigmatism) 107안에 토릭 소프트 콘택트렌즈를 착용시켰다. 눈 깜박임에 따른 렌즈 회전 변화 양상과 주시 방향 변화 또는 렌즈를 45° 회전시킨 후 1분 동안의 렌즈 회전 패턴을 평가하였다.
정면 주시 시 각막 지형에 따라 토릭 렌즈의 축 회전량에는 통계적으로 유의한 차이가 나타났으며, 비대칭나비형 각막에서 가장 큰 회전량을 보였다. 대각선방향 주시 시에는 모든 각막 지형에서 회전량의 유의한 차이가 관찰되었으나, 수평 주시에서는 타원형 각막에서만 유의한 차이가 나타났고, 대칭 및 비대칭나비형 각막에서는 수직 주시에서만 유의한 차이가 확인되었다. 렌즈를 귀쪽 방향으로 45° 임의 회전시킨 경우 각막 지형 간 회전 양상에는 차이가 없었다. 반면, 코쪽 방향으로 회전시킨 경우 45초까지는 차이가 없었으나, 45–60초 구간에서는 각막 지형에 따른 차이가 관찰되었다.
각막 지형은 토릭 소프트 콘택트렌즈의 회전량에 영향을 미치는 요인으로 확인되었으며, 최적의 축 안정성을 확보하기 위해 렌즈 피팅 시 각막 형태를 고려할 필요가 있음을 제안한다.
Keywords:
Lens rotation, Corneal topography, Recovery rate, Toric soft contact lens, With-the-rule astigmatism키워드:
회전량, 각막지형도, 회복률, 토릭소프트콘택트렌즈, 직난시Introduction
The use of toric soft contact lenses to correct astigmatism has become increasingly common, and research continues to investigate the effects of corneal shape on toric lens fitting.[1-3] In Asian markets, the rate of toric lens prescriptions in Japan increased from 6% to 12% between 2003 and 2016,[4] and in 2018, a study of adolescents in China found that around 60% of subjects had astigmatism[5]; thus, the demand for toric lenses is expected to continue to grow in Asian markets. Unlike spectacles, contact lenses correct visual acuity through direct contact with the cornea; thus, the position of the lens center can be altered by blinking or shifts in gaze direction.[6-8] In particular, the rotation of toric lenses on the eyeball leads to refractive abnormalities that can result in blurring, decreased visual acuity, and eye strain caused by the lens.[7] For this reason, soft toric lenses possess unique designs to provide axial stability, in order to maintain a consistent orientation and effectively correct vision despite movements during wearing. The basic stabilizing designs of soft toric lenses include prism-ballast designs, in which a prism is placed in the lower part of the lens, as well as dynamic stabilization designs, in which the eyelids cover the thin upper and lower parts of the lens. As a result, the thicker central portion of the lens is placed horizontally between the eyelids to provide stability.[6-8]
The movement of soft toric lenses is known to be affected by the lens design, settling time, blinking, degree of myopia, palpebral aperture, and several angles of the lid anatomy.[8,9] However, due to the diversity of subjects and criteria used to evaluate the rotational stability of toric lenses, it is difficult to compare data between studies.[1-3]
Corneal topography, which uses placido disc reflection to examine the refractive power and radius of the curvature of the anterior surface of the cornea, is the most basic means of measuring corneal shape. The height of corneal sections can be measured using a Scheimpflug camera combined with topography. These measurements can then be used to visualize the corneal shape by using different colors to represent the refractive power of the corneal surface. Maguire et al.[10] and Gormley et al.[11] developed a classification of sagittal topography maps, and Bogan et al. [12] later simplified this classification into five shapes: round, oval, symmetric bowtie, asymmetric bowtie, and irregular. Currently, the classification criteria of Bogan et al. are still used in research to classify corneal shape in specific groups or races and to test aberrations or perform optical quality analysis for dry eye syndrome.[13,14]
Research is being conducted to elucidate the correlations between contact lens fitting and the refractive power of the steep and flat principal meridians of the cornea, which can be checked with a keratometer that only measures the central part of the cornea, as well as corneal eccentricity, the degree of astigmatism and refractive power of the anterior and posterior surfaces of the cornea, corneal height, and anatomical characteristics of the corneal limbus, which can all be measured by corneal topography.[1-3] Thus, a large number of studies have been conducted regarding the use of corneal topography measurements for contact lens fitting. However, there have not yet been any studies on the effects of differences in corneal shape on soft toric lenses using the Bogan classification method, which classifies the topography via qualitative evaluation of color-coded topographic maps.
Therefore, this study aimed to investigate the effects of corneal shape on the direction and amount of rotation of toric soft lenses, on the amount of rotation according to gaze direction, and on the rate of recovery from rotation. This study presents an additional corneal factor to be considered in fitting guidelines for soft toric lenses.
Methods
1. Subjects and study design
Participants in this study were aged 20–39 years. They had no history of ophthalmologic disease or surgery and had with-the-rule astigmatism (Axis: 180±15°) with a total astigmatism of at least -0.75 D by objective refraction test. Based on these criteria, a total of 61 subjects were selected (39 males, 22 females; mean age: 23.21±2.48 years). The direction and amount of rotation, and the amount of rotation depending on gaze direction measurements were obtained in 114 eyes (8 eyes were excluded based on the astigmatism criteria). However, in the classification of corneal shape, round (4 eyes) and irregular (3 eyes) shapes were much less common than the other categories and were therefore excluded, leaving 107 eyes in the analysis.
This study was conducted in accordance with the tenets of the 1964 Declaration of Helsinki and its later amendments and was approved by an institutional review board designated by the South Korea National Institute for Bioethics Policy (approval number: P01-201808-11-001). Informed consent was obtained from participants prior to study inclusion.
2. Assessment of toric lens rotational movements
After wearing soft toric lenses (accelerated stabilization design [ASD], 1-day Acuvue® moist lenses for astigmatism) and waiting 15 min for stabilization, rotational movements were recorded using a video camera (VPC-SH1, SANYO, Japan). Corneal radius (K values mean±SD : 8.01±0.28, 95% CI: 7.959~8.067) was measured prior to lens fitting. The toric lenses used in this study were manufactured with a single base curve, and fitting was performed according to the manufacturer’s recommended guidelines. Using Photoshop software (Adobe Photoshop 7.0.1, Adobe Systems Incorporated, United States) recorded videos, the direction and extent of rotation were measured based on the axial mark on the soft toric lenses (6 o’clock direction). The amount of rotation for different gaze directions was assessed relative to the rotation during primary gaze after wearing the lenses. First, toric lens axis position was measured at primary gaze. After that, the subject was instructed to look at another direction and blink 3 to 4 times naturally. This process was repeated for 8 different directions, separated by intervals of 45° in the clockwise direction, starting from 12 o’clock. When the gaze direction was changed, the subject was asked to blink naturally while staring at the target in primary position to minimize the influence of the previous measurement. The order of gaze direction was randomly determined.[7] The rate of recovery from rotation was analyzed by recording recovery movement towards the original axis during 1 min after inducing an arbitrary rotation of the lens of 45° in the temporal and nasal directions. To describe the reorientation process more intuitively, the angular rotation was converted into linear displacement (mm) along the lens surface using the arc length formula (s=rθ), where r represents the lens radius and θ represents the rotation angle in radians.
For measurement of the rate of recovery from rotation, 23 of 107 eyes were excluded because they exceeded the 5° range of rotation suggested in the manufacturer’s guidelines when measuring rotation in primary gaze, or because they were affected by unstable blinking and eyelid tension in either gaze direction (temporal direction, 3 eyes; nasal direction, 1 eye); hence, 84 eyes were selected for the rotation analysis. (Oval : 21 eyes, Symmetric bowtie : 48 eyes, Asymmetric bowtie : 15 eyes)
3. Statistical analysis
In order to compare fitting (amount of rotation, rotation rate) between corneal shapes, the normality of the data was first tested (Shapiro–Wilk test, Kolmogorov–Smirnov test, SPSS ver.18, USA). Since some of the corneal shape groups did not satisfy the conditions of normality, the non-parametric Kruskal-Wallis test and post-hoc Bonferroni correction method was used. In all cases, a p-value < 0.05 was considered statistically significant.
Results
1. Direction and amount of rotation in primary gaze
When the mean direction of rotation was analyzed for different corneal shapes in primary gaze, compared to oval-shaped corneas, symmetric bowtie-shaped corneas showed a stronger tendency to rotate temporally (Table 1). For asymmetric shaped corneas, which have the least symmetry, the direction of rotation was also analyzed according to the location of the point with the steepest curvature. When the steepest curvature was superior to the horizontal midline of the cornea, the ratio of nasal vs. temporal rotation was around 6:4. However, when the steepest curvature was inferior to the horizontal midline, the ratio was 1:9, showing a much higher rate of rotation towards the temporal direction (Table 1).
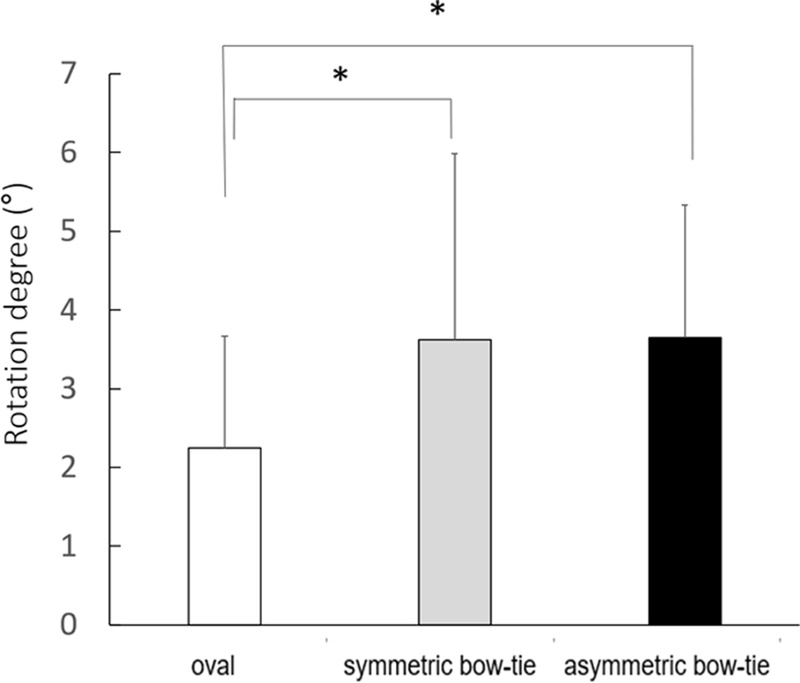
When the amount of temporal or nasal lens rotation relative to the 6 o’clock direction was analyzed irrespective of the direction, there were statistically significant differences in the amount of rotation depending on the corneal topography (p=0.024, Fig. 1). In the analysis by corneal topography group, the oval shape showed significant differences with the symmetric and asymmetric bow tie shapes in the amount of rotation (post-hoc test-bonferroni correction method, p=0.016 and 0.011, respectively), with the oval shape showing the least rotation of the three groups. There was no statistically significant difference in the amount of rotation between the symmetric and the asymmetric bowtie shapes.
2. Stable position and rate of recovery during 60 s after arbitrary lens rotation
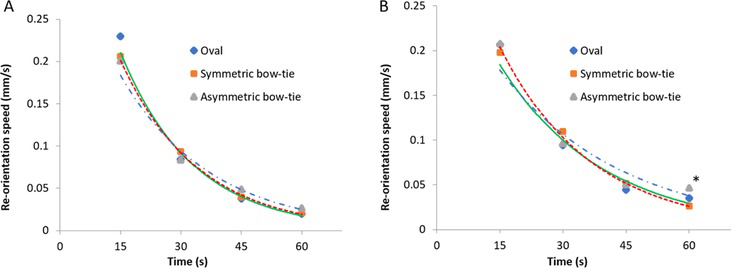
With the subject wearing the lens, the lens was rotated 45° temporally, and after natural blinking for 60 s, the stable position of the lens differed significantly depending on the corneal shape. After 60 s, the position of the lens axis stabilized at 3.28±3.48° off-center for ovals, 4.69±4.71° for symmetric bowties, and 6.53±4.32° for asymmetric bowties, meaning that corneal topography was associated with differences in the stable position after arbitrary rotation in the temporal direction (p=0.046, Fig. 2A). Similarly, statistically significant differences were observed in the axial orientation depending on corneal topography 60 s after nasal rotation (p=0.026, Fig. 2B). Following nasal or temporal rotation, among all three groups, there were statistically significant differences in the stable position between the oval-shaped cornea group and the asymmetric bowtie-shaped cornea group (post-hoc test, respectively temporal p=0.043, nasal p=0.020). In contrast, the symmetric bowtie-shaped cornea group showed no differences in the stable position compared with the oval-shaped cornea group or the asymmetric bowtie-shaped cornea group, in either direction (p>0.05). Following an arbitrary rotation of the lens in the temporal direction, the rate of rotation was investigated across four intervals for 60 s (Table 2). The slope of the trend line showing the rate of rotation by interval was the steepest for oval-shaped corneas, followed by symmetric bowtie-shaped corneas, then asymmetric bowtie-shaped corneas, but there were no statistically significant differences in any interval. Following arbitrary rotation in the nasal direction, there were no differences in the rate of lens rotation between cornea shapes from 0 to 45 s, but in the final 45–60-s interval, the asymmetric bowtie group showed a significantly faster rate of rotation than did the oval group (Fig. 3, Table 2).
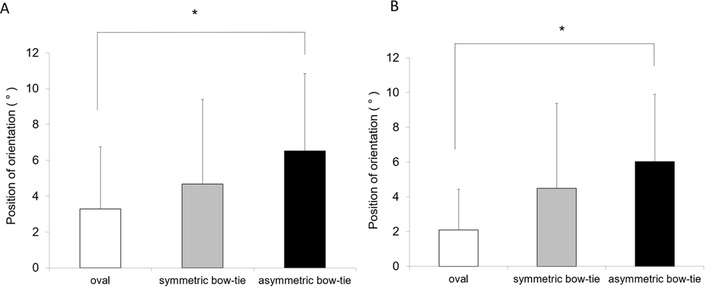
Stable position and rate of recovery during 60 s after arbitrary lens rotation. A Temporal direction. B Nasal direction. (Error bars represent the standard deviation)

Lens-reorientation speed after 45° dislocation in the temporal or nasal direction based on corneal type(mm/s)
3. Amount of lens rotation for different gaze directions
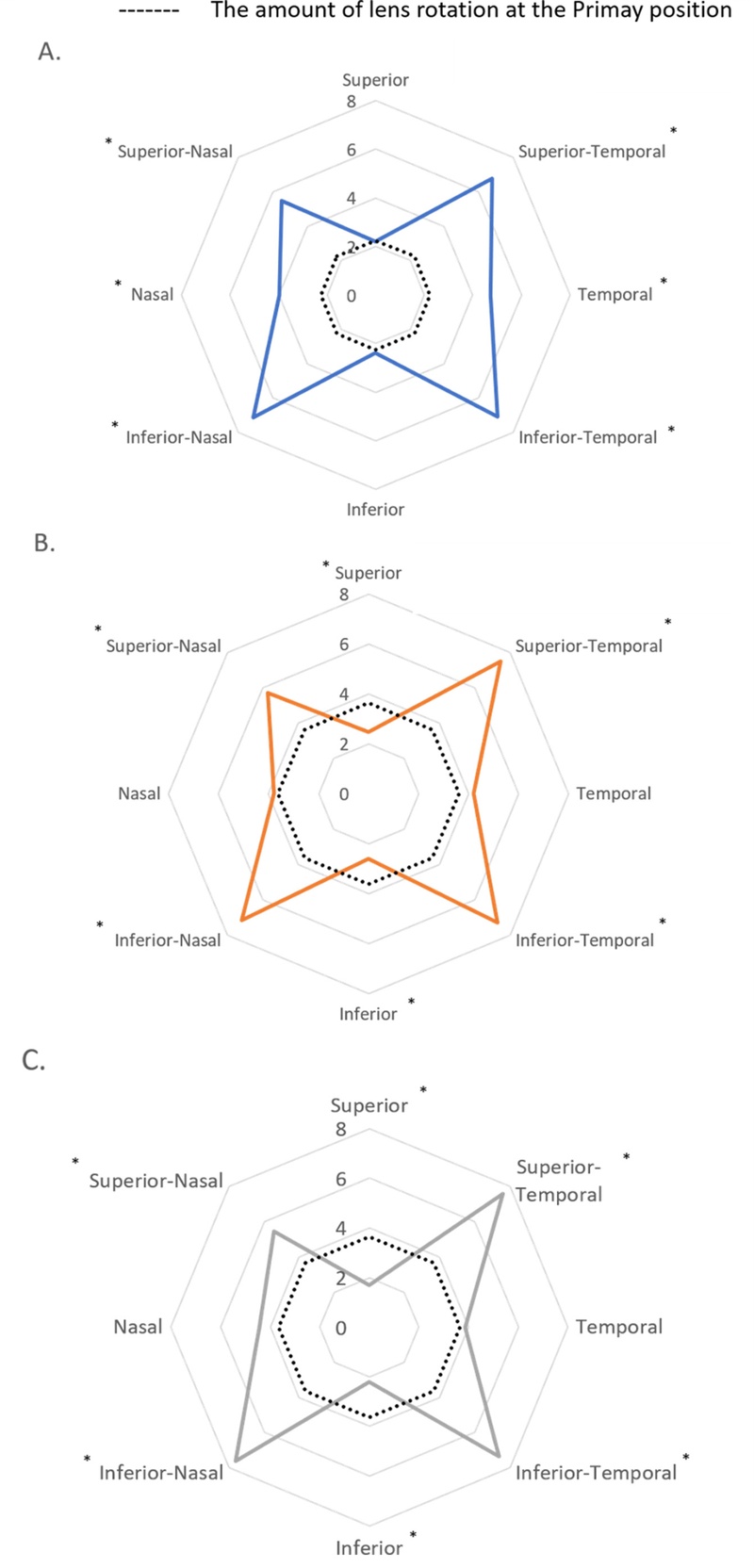
While wearing soft toric lenses, when subjects changed the direction of their gaze in the four vertical and horizontal directions (superior, inferior, nasal, temporal) and the four diagonal directions, there were no significant differences in the stable axial orientation according to corneal topography (p>0.05). When the amount of lens rotation was compared between the eight directions of gaze and primary gaze in each topography group, all groups showed a significant increase in rotation for the four diagonal directions of gaze (Fig. 4A-C). In Fig. 4, the dashed line represents the amount of lens rotation at primary gaze, whereas the colored solid lines indicate the magnitude of axis rotation at each gaze direction. When gaze was directed vertically upwards or downwards, the symmetric and asymmetric bowtie groups showed significantly decreased rotation compared to primary gaze (symmetric bow tie and asymmetric bow tie groups, superior and inferior directions, all p<0.05). Meanwhile, the oval group showed no significant differences between primary gaze and gaze in the vertical directions but showed significantly increased rotation for gaze in the horizontal directions, temporal and nasal, compared with primary gaze (temporal p=0.033, nasal p=0.046).
Discussion
This study analyzed rotational movements of toric lenses during primary gaze and altered directions of gaze in groups with different corneal topography. During primary gaze, the oval group showed the smallest angle of displacement, followed by the symmetric bow tie-shaped group, and the asymmetric bowtie-shaped group. Likewise, when the stable position of the lens was analyzed in relation to corneal shape a certain time after arbitrary rotation, the oval group showed the least amount of displacement.
This study revealed fitting patterns for different corneal shapes using ASD toric lenses. For the ASD, the upper and lower parts of the lens are made thinner, and four additional stabilization zones are included in the central part of the lens to reduce rotation of the lens on the corneal surface. In previous studies on the efficacy of this type of lens design, toric lenses with ASD were reported to be more stable, in terms of axial rotation, than lenses with a prism-ballast design.[15-17] McIlraith et al.[7] observed differences in the amount of rotation during primary gaze when standing or lying between four types of toric lens with different stabilization designs and demonstrated that the gravity acting on the lens affected rotation. In addition, when standing, shifted gaze direction showed different amounts of rotation compared to primary gaze, and thus it was proposed that the shape of the upper and lower eyelids could affect lens rotation. In this study as well, the amount of rotation during primary gaze was 2.24±1.42° for the oval group, 3.62±2.36° for the symmetric bowtie group, and 3.46±1.67° for the asymmetric bowtie group. These ranges are comparable with those reported by Hickson-Curran et al.[2] using lenses with the same axial stabilization design.
In these results, during primary gaze, the stable position of the axis marker on the lens was found to be on the nasal side in around 10% more subjects in the oval group only, while the stable position of the lens was more frequent in the temporal direction in the other two groups. In a previous study of Chinese individuals using toric lenses with the same stabilization design, the lens axis was found to be oriented in the inferior-temporal direction.[2] Although the previous study did not investigate the stable position for different corneal topographies, our results were similar to those reported in that study.
Inducing arbitrary rotation of the lens axis and observing lens movements due to natural blinking is an established method of assessing the efficiency of axial recovery in toric lenses.[18] The amount of arbitrary rotation differs between studies, usually in the range of 30–60°[18]; referring to past research, the present study tested rotational stability of the lenses using the middle value of 45°. In a study by Tan et al.,[19] following arbitrary rotation of toric lenses 30° in the temporal or nasal direction, recovery was measured after 10 blinks, and differences between different lens designs were investigated. There were no differences in stability according to design, and the mean recovery was equal or better for nasal rotation. Young et al.[16] observed recovery rates of 22–25°/min after arbitrary rotation of 45°. In this study, after rotation of the lenses, the recovery rate was observed for 1 min, and the mean recovery rate was 44.18°/min, which was faster than the rate reported in the abovementioned previous study. However, this 2-fold difference in recovery rate can be explained by the fact that in the previous study, the rotation was monitored over a period of 3 min, whereas in the present study, recovery was only compared in the first minute. When the 1-min recovery period was subdivided into four 15-s intervals, there was an approximately 50% decrease in the recovery rate from the first to the second interval, as well as from the second to the third, and from the third to the fourth interval. Thus, following arbitrary rotation of toric lenses, the recovery rate was the fastest immediately after rotation.
The stability of toric lenses is usually assessed in forward gaze (primary position), but it has been proposed that rotation needs to be assessed in various directions of gaze to provide an assessment that better reflects daily living.[7] In the present study, in order to assess the stability of the lenses from multiple angles, in addition to the primary position, rotation was measured when subjects shifted their gaze up, down, left, right, or diagonally. Differences in rotation were observed according to gaze direction, even within the same subjects. This is consistent with the findings of a previous study by Roberta et al.,[7] in which rotation was reported to increase for gaze in diagonal directions compared with vertical or horizontal gaze. Notably, the previous study only found increased rotation in upward diagonal gaze, while a significant increase was also observed in rotation for downward diagonal gaze in this study; this discrepancy could be the result of racial characteristics of the subject group (Caucasian and Asian), such as the size and shape of the palpebral fissure, or the angle of the eyelids. Although many studies have been conducted on the fitting characteristics of toric lenses, results on rotational stability of different toric lens designs have shown inconsistencies depending on the study conditions, subjects, or variables of interest, and thus it can be surmised that the anatomical characteristics of the wearer can affect the fit of toric lenses.[8]
Previous research has investigated the relationship between corneal topography measurements and soft lens fitting in order to identify factors other than lens stabilization design that could affect lens rotation.[1,20] Young et al.[1] reported that compared with methods using a keratometer, soft lens fitting could be better predicted using measurements such as corneal curvature and eccentricity, which can be measured by placido ring-based corneal topography. Similarly, in a study by Sheila et al.,[2] soft contact lens fitting was assessed by measuring Chinese and Caucasian ocular topographs and anatomical dimensions of the anterior segment, whereby factors such as palpebral fissure size and horizontal visible iris diameter were reported to affect fitting. Although there are prior studies on Chinese toric contact lens fitting, we consider our study to be meaningful as it is the first study to classify corneal topography in Koreans and to observe the movement of contact lenses accordingly.
To our knowledge, limited research has examined the relationship between corneal topography classified by the method of Bogan et al.[12] and soft toric lens fitting. Asymmetric bowtie-shaped corneas, which have relatively high irregularity within the Bogan classification system, showed greater lens rotation in primary gaze and greater displacement following recovery after arbitrary lens rotation than did both oval-shaped and symmetric bowtie-shaped corneas. Although corneal irregularity has been studied as a factor affecting lens fitting,[21] the oval, symmetric bowtie, and asymmetric bowtie groups in this study did not show any significant differences in astigmatism or eccentricity of the cornea. When the direction of gaze was changed, for horizontal gaze, oval-shaped corneas showed increased rotation compared with primary gaze, but this was not observed for symmetric and asymmetric bowtie-shaped corneas. Oval-shaped corneas show greater convexity in the horizontal direction compared with symmetric and asymmetric bowtie-shaped corneas. When the direction of gaze is shifted, the lens moves on the cornea, and the lens fit may be affected by changes in the convexity of the corneal meridians. This study has several limitations, including the lack of evaluation of the optical effects of the rotation of the contact lens. In addition, various toric contact lens stabilization designs were not evaluated. Therefore, there may be limitations in applying the results of this study to toric lenses of different designs from those used in this study. Furthermore, factors such as eyelid tension, dry eye conditions, and variations in tear volume, which may influence contact lens rotation and stability, were not evaluated in this study. In addition, because data from both eyes of some subjects may have been included in the analysis, the assumption of independence between observations could have been violated, and the results should therefore be interpreted with caution. Further studies in the area of toric lens rotation using a variety of stabilization designs will help to elucidate the relative importance of corneal topography or curvature of the cornea for subjects adopting a variety of gaze directions. Future work could also assess optical performance, including visual acuity and aberrometer of the eye in a variety of gaze directions.
Conclusions
This study compared the fitting of toric lenses based on color maps expressing the curvature measured by corneal topography. The overall corneal topography affects the movement of toric lenses, and these differences can, in turn, affect the wearer’s comfort and visual correction. Therefore, this study suggests that corneal shape should be considered when prescribing toric lenses.
References
-
Young G, Schnider C, Hunt C, et al. Corneal topography and soft contact lens fit. Optom Vis Sci. 2010;87(5):358-366.
[https://doi.org/10.1097/OPX.0b013e3181d9519b]

-
Hickson-Curran S, Young G, Brennan N, et al. Chinese and Caucasian ocular topography and soft contact lens fit. Clin Exp Optom. 2016;99(2):149-156.
[https://doi.org/10.1111/cxo.12336]

-
Macedo-de-Araújo RJ, Amorim-de-Sousa A, Queirós A, et al. Relationship of placido corneal topography data with scleral lens fitting parameters. Cont Lens Anterior Eye. 2019;42(1):20-27.
[https://doi.org/10.1016/j.clae.2018.07.005]

-
Itoi M, Itoi M, Efron N, et al. Trends in contact lens prescribing in Japan (2003-2016). Cont Lens Anterior Eye. 2018;41(4):369-376.
[https://doi.org/10.1016/j.clae.2018.02.001]

-
Chen Z, Liu L, Pan C, et al. Ocular residual and corneal astigmatism in a clinical population of high school students. PLoS One. 2018;13(4):e0194513.
[https://doi.org/10.1371/journal.pone.0194513]

-
Tomlinson A, Ridder WH 3rd, Watanabe R. Blink-induced variations in visual performance with toric soft contact lenses. Optom Vis Sci. 1994;71(9):545-549.
[https://doi.org/10.1097/00006324-199409000-00001]

-
McIlraith R, Young G, Hunt C. Toric lens orientation and visual acuity in non-standard conditions. Cont Lens Anterior Eye. 2010;33(1):23-26.
[https://doi.org/10.1016/j.clae.2009.08.003]

-
Momeni-Moghaddam H, Naroo SA, Askarizadeh F, et al. Comparison of fitting stability of the different soft toric contact lenses. Cont Lens Anterior Eye. 2014;37(5):346-350.
[https://doi.org/10.1016/j.clae.2014.05.003]

-
Young G, Hunt C, Covey M. Clinical evaluation of factors influencing toric soft contact lens fit. Optom Vis Sci. 2002;79(1):11-19.
[https://doi.org/10.1097/00006324-200201000-00008]

-
Maguire LJ, Singer DE, Klyce SD. Graphic presentation of computer-analyzed keratoscope photographs. Arch Ophthalmol. 1987;105(2):223-230.
[https://doi.org/10.1001/archopht.1987.01060020077033]

- Gormley DJ, Gersten M, Koplin RS, et al. Corneal modeling. Cornea. 1988;7(1):30-35.
-
Bogan SJ, Waring GO 3rd, Ibrahim O, et al. Classification of normal corneal topography based on computer-assisted videokeratography. Arch Ophthalmol. 1990;108(7):945-949.
[https://doi.org/10.1001/archopht.1990.01070090047037]

-
Mirzajani A, Aghataheri S, Ghoreishi M, et al. Evaluation of corneal higher order aberrations in normal topographic patterns. J Curr Ophthalmol. 2016;28(2):75-80.
[https://doi.org/10.1016/j.joco.2016.03.001]

-
John T, Tighe S, Sheha H, et al. Corneal nerve regeneration after self-retained cryopreserved amniotic membrane in dry eye disease. J Ophthalmol. 2017;2017:6404918.
[https://doi.org/10.1155/2017/6404918]

-
Zikos GA, Kang SS, Ciuffreda KJ, et al. Rotational stability of toric soft contact lenses during natural viewing conditions. Optom Vis Sci. 2007;84(11):1039-1045.
[https://doi.org/10.1097/OPX.0b013e318159aa3e]

-
Young G, McIlraith R, Hunt C. Clinical evaluation of factors affecting soft toric lens orientation. Optom Vis Sci. 2009;86(11):E1259-E1266.
[https://doi.org/10.1097/OPX.0b013e3181bc63b4]

-
Forister JFY, Chao J, Khy K, et al. Predicted tear layer oxygen tensions under two designs of silicone hydrogel toric lenses. Cont Lens Anterior Eye. 2008;31(5):228-241.
[https://doi.org/10.1016/j.clae.2008.06.003]

-
Edrington TB. A literature review: the impact of rotational stabilization methods on toric soft contact lens performance. Cont Lens Anterior Eye. 2011;34(3):104-110.
[https://doi.org/10.1016/j.clae.2011.02.001]

-
Tan J, Papas E, Carnt N, et al. Performance standards for toric soft contact lenses. Optom Vis Sci. 2007;84(5):422-428.
[https://doi.org/10.1097/OPX.0b013e318059063b]

-
Hall LA, Young G, Wolffsohn JS, et al. The influence of corneoscleral topography on soft contact lens fit. Invest Ophthalmol Vis Sci. 2011;52(9):6801-6806.
[https://doi.org/10.1167/iovs.11-7177]

-
Young G, Hall L, Sulley A, et al. Inter-relationship of soft contact lens diameter, base curve radius, and fit. Optom Vis Sci. 2017;94(4):458-465.
[https://doi.org/10.1097/OPX.0000000000001048]